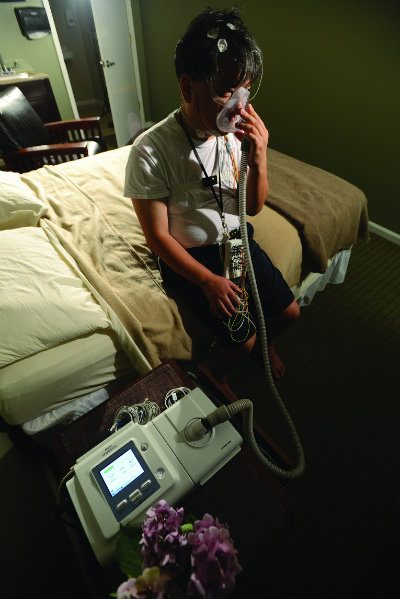
Dealing with obstructive sleep apnea (OSA) requires an understanding of the causes, symptoms and potential cures. But while diagnosis is relatively straightforward after one sleep study, getting patients to comply with their treatment regimen often proves difficult.
Numerous factors contribute to the development of OSA, including gender, weight, age and race. All relate to the probability of the airway collapsing while horizontal, which interferes with breathing. Men are more likely to develop OSA than women, in part because estrogen helps keep palate muscles strong. After menopause, women’s risk increases. In fact, the risk for both sexes increases with age, since people over 60 are more susceptible to weight gain and loss of muscle tone. Being overweight—at any age—can cause wider necks, recessed chins and larger tongues, narrowing the airway passage and creating a blockage when lying down. Because of facial structures, certain races are more prone to develop sleep apnea at lower body weights, including those of Asian descent—like Jack Li. Narcotics and sedatives, including alcohol, painkillers and sleep aids like Ambien, relax throat muscles and make sleep apnea worse.
Each time breathing stops, the brain experiences an arousal, or an interruption from sleep. This means it’s impossible for someone with sleep apnea to complete a restorative sleep cycle. Anyone who has pulled an all-nighter or had a particularly rough night of sleeping has felt the symptoms of sleep deprivation the following day: irritability, difficulty concentrating, mood swings and memory problems. And that’s just after one night.
For sleep apnea sufferers, these adverse cognitive symptoms are usually accompanied by high blood pressure (hypertension), which creates a higher risk for cardiovascular events like stroke and congestive heart failure. Sleep apnea tends to go hand in hand with conditions like type II diabetes and emphysema.
Despite these dramatic health problems, the compliance rate of sleep apnea treatment among Americans is roughly 50 percent, meaning half of all diagnosed patients never follow through with using CPAP or an oral appliance. To many, it seems too inconvenient, too uncomfortable, or too embarrassing.
READ MORE: Learn about snoring in “The ABCs of ZZZ’s”
In 2009, Dr. Marc Benton and a colleague, Neil Friedman, led a study that revealed a creative way to motivate men to use CPAP. Doctors typically give their patients a long list of ailments that will improve after using CPAP, from hypertension to headaches and heart problems. “[For] a lot of people, that doesn’t matter,” says Benton. On the other hand, tell the same patients their golf game will improve, and all of a sudden they are inspired to stick with the program. Benton and Friedman selected 12 golfers with sleep apnea who had never used CPAP or gave up. Over the course of three to five months of obligatory CPAP use, the golfers lowered their handicaps by as much as three strokes. The impressive results were cited in the 2014 Fitness Issue of Golf Digest. “We like to think of ourselves as CPAP whisperers,” says Friedman. “We get people to use it. Our [compliance] rate is 80 percent.”
The beauty of the golf study is that factors affecting golfers’ handicaps are also desirable in regular life: endurance, strategy, anger management, memory, decision-making, reaction time and focus. “These are qualities that are no different than what’s important for you to function at work,” Benton explains. “A handicap is an incredibly strong predictor of performance, [and] it is reasonable to assume that if you had a way of measuring job functionality, you’d see the same improvement after treatment.”
Other patients require a different motivator. “You tell people they’ll be better socially—for certain people, that makes a big difference,” Benton adds.

CPAP therpay does come with a fair share of challenges. It is hard for most people to grasp the concept that they will be sleeping with this kind of device for the rest of their life. I found out that i had sleep apnea a couple years back and i intially felt the same way. The fact that i would have to wear this mask at night really discouraged me from my “sexy time.” But in, time, CPAP mask becomes bearable, and you learn to adjust your life to it. The benefits that you see when you wake up refreshed in the morning and full of energy make it all worth it. My advice is to bear through it.