
Daniel Fernandez knew from the time he was about 5 that he was a boy being raised as a girl. “I always had an inkling that I was a male,” says Fernandez, now 32. “In college I came to terms with my gender identity and started transitioning socially.”
At 25, Fernandez made the decision to transition medically. With few health care resources for LGBTQ individuals in New Jersey at the time, Fernandez traveled from his home in Highland Park to a clinic in Philadelphia, where he received hormonal treatment and gender-affirming surgeries.
While Fernandez was transitioning, routine medical visits at various local facilities were unpleasant. Waiting to discuss the results of an ultrasound for stomach issues, he was harangued by another patient. “The receptionist did nothing to help,” Fernandez says. “I walked out and never did get the results.” Another time, at an urgent care facility for a physical exam, a nurse asked unnecessarily intrusive questions.
“These experiences had a negative impact emotionally,” Fernandez recalls. “Many times, I put off or avoided doctor visits because of the harassment I experienced.”
[RELATED: Top Doctors 2021]
Then, in 2017, Fernandez started going to the Robert Wood Johnson University Hospital Somerset Babs Siperstein PROUD Center. “It was definitely a relief, a breath of fresh air, to be in an office that is inclusive and asks which pronoun you prefer. When I saw the [Pride] flag in the waiting room, I felt welcomed and safe.”
Fernandez now works at the Robert Wood Johnson University Hospital PROUD Gender Center of NJ as co-facilitator of the Proudly Me Education Support Group and as a health navigator, welcoming patients and explaining the center’s resources.
According to Garden State Equality, New Jersey’s largest LGBTQ advocacy group, there are about 500,000 LGBTQ people in New Jersey. Yet it wasn’t until recently that these New Jerseyans could find conveniently located health care practices that welcomed them. Now, a growing number of such facilities have emerged throughout the state, spurred by cries for providers to show respect for diversity.
“For far too long, LGBTQ individuals had to travel to Philadelphia or New York City to feel comfortable about their health care needs,” says Christian Fuscarino, executive director of Garden State Equality, which provides sensitivity training to primary care physicians in all 21 New Jersey counties. “We helped pave the way for providers to be more competent with LBGTQ health issues.”
Insensitivity at the doctor’s office takes various forms, ranging from outright bias to lack of interest or knowledge. “A transgender individual visiting a primary care physician or endocrinologist may find that the doctor is not as informed about this group’s health care needs, such as surgery or hormones,” says Cathy Renna, communications director at the National Gay and Lesbian Task Force. “Other physicians may be insensitive or hostile to LGBTQ patients, who then fear walking into a doctor’s office, concerned that they won’t be respected, understood or treated properly.” People of color within the LGBTQ community have added concerns about bias. “These are marginalized communities within other marginalized communities,” says Fernandez.

Dr. Justin Schweitzer is medical director of LGBTQ+ Health and Primary Care at Cooper Alliance in Cherry Hill, which opened in 2020. Photo by Landon Spears
“Fifty percent of people who identify as LGBTQ have experienced some form of health care discrimination, intentional or not,” says Dr. Justin Schweitzer, medical director of LGBTQ+ Health and Primary Care at Cooper Alliance in Cherry Hill. “It’s not that providers are trying to hurt the patient. It’s that they’re not going above and beyond and don’t know much about health care issues of the LGBTQ community.” The practice opened in 2020 in response to LGBTQ needs.
Finding a knowledgeable and sensitive provider isn’t easy. But Gabriel (who asked to use only his first name) was lucky. Now 29, Gabriel was living in Kearny when, at 18, he identified as gay. “There were a limited number of doctors who welcomed gay men at that time,” he says. “… They didn’t ask many questions, didn’t inform me about risks, and never recommended HIV testing.”
Gabriel found out about HIV testing when he was at a bar where a mobile unit from the North Jersey Community Research Initiative (NJCRI) in Newark stopped by. He now does field testing and is an HIV counselor for NJCRI.
Eileen Scarinci works as a nurse practitioner while Gabriel (who asked us to use only his first name) is an HIV counselor and does field testing for North Jersey Community Research Initiative, which treats 10,000 people each year. Photo by Landon Spears
No matter how LGBTQ patients identify, they are typically at increased risk for HIV and sexually transmitted diseases. “We see a large number of patients with sexually transmitted diseases—gonorrhea, syphilis and chlamydia,” says Eileen Scarinci, a nurse practitioner at NJCRI, which treats 10,000 people a year, half of them from the LGBTQ community. “We’re preventing the transmission of HIV with PrEP (HIV prevention medication), but that opens the door for STDs as people treated with PrEP feel it’s safe to start engaging in unprotected sex.”
At NJCRI, which began as an AIDS-research facility 33 years ago, no one, including uninsured people and undocumented immigrants, is turned away. “The initiative is a diamond in the rough, the best-kept secret in Essex County,” says Scarinci.
***
When an LGBTQ individual finds the right provider or practice, the experience can be life changing. That was the case for Kai Samantha Ingram, 31. As a 5-year-old assigned male at birth, Ingram didn’t feel comfortable with her gender. She didn’t like boys’ activities or clothing. As she grew older, she would paint her nails and walk around in her mother’s wedges.
“Beginning when I was 18, I wore women’s clothes for special occasions and then all the time,” she says. At that point, she began thinking about transitioning medically, but she couldn’t find any doctors in New Jersey and didn’t want to travel to New York. “Transitioning was on my mind every day,” she says. “I felt I had to make a decision, but there was no doctor around to help.”
After several years of worry, Ingram heard from a friend who recommended Dr. Michelle Dalla Piazza, associate director of the Transgender Health program at the Infectious Diseases Practice at Rutgers-Newark. “I was so ecstatic,” says Ingram, who had hormone-replacement therapy, breast implants and gender-affirming surgery. “Dr. Dalla Piazza made me feel better about myself.”
The Infectious Diseases Practice, initiated in 2017, cares for LGBTQ+ patients across the spectrum. The program offers services such as hormone treatment, mental health care and counseling, sexual health care and referrals for gender-affirming surgery and primary care.
The transgender program began with 10 patients. Now there are more than 200. “We took many steps to ensure that our patients would feel welcome,” says Dalla Piazza. “Many of our patients tell us that they don’t necessarily want to be singled out by going to a space exclusively dedicated to transgender health, so we provide our services in a gender-neutral way, meaning that our transgender patient appointments are interspersed with all other appointments.”
***
Trying to find a welcoming provider can be a challenge even for someone like Kristen Krause, 31, the deputy director of the Center for Health, Identity, Behavior and Prevention Studies at Rutgers. While in graduate school, Kristen began figuring out her sexual identity and at 18 identified as lesbian. At that time, she used her college’s health services. After college she saw a primary care doctor. “I have a feminine presentation,” says Krause. “Doctors assumed I was straight, and since they asked no questions, I said nothing to correct them.” Now, she says there’s a move for doctors to inquire about the patient’s relationships and sexual identity and address a patient’s mental as well as physical health. When Krause moved from New York City to New Jersey in 2017, she started looking for a health care provider. She’s still seeking a facility that is LGBTQ friendly, with a provider asking questions about sexual orientation and pronoun preference.
“It all comes down to cultural competence, an understanding of how an individual’s different aspects, including gender and ethnicity, affect health and well-being,” says Krause.
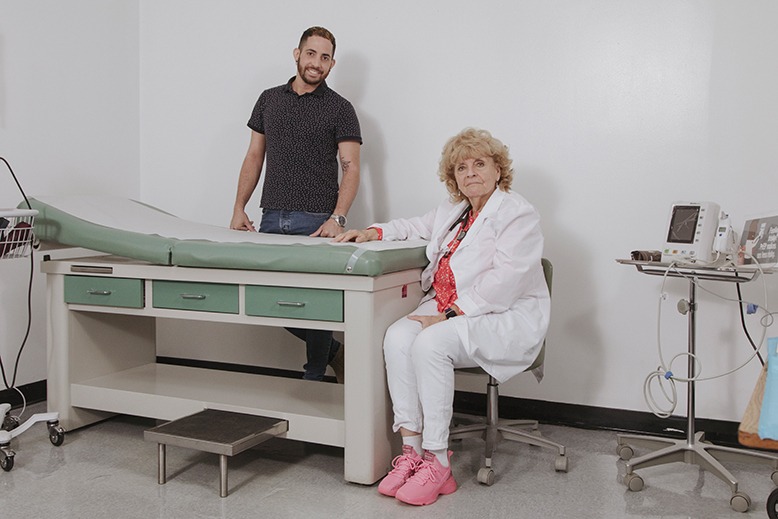
“One of the issues, absolutely, is insensitivity, not being responsive to the individual,” says Dr. Gloria Bachmann, medical director of the PROUD Gender Center of New Jersey. “When a transgender individual’s name and genitalia don’t match, they may not get optimal care,” she says. Or they may avoid or delay care or go to an inappropriate provider.
“Many LBGTQ patients are reluctant to seek care unless it’s an emergency, so they will stay home and deal with the problem or go where they’ll get substandard care,” says Bachmann, noting that the center, founded in 2020, is designed to respond to the need, not only for clinical services, but also for education for patients and their families.
For Dr. Juana Hutchinson-Colas, director of Female Pelvic Medicine and Reconstructive Surgery at the center, education is an important component of treating transgender men who want to medically transition. “They will receive testosterone therapy for at least a year, and live in male gender roles for a year and we’ll discuss whether to remove or keep the ovaries,” explains Hutchinson-Colas, “but it is the patient’s decision. My job is providing information about benefits and risks.”
In striving for greater sensitivity, some practices are modifying their intake forms, asking which pronoun the patient prefers, and displaying empowering messages in waiting rooms. “After the AIDS epidemic, the medical establishment realized where they did well and where they fell down,” says Renna, of the National Gay and Lesbian Task Force. “There’s a new understanding of who we are, and more advocacy, education and sensitivity training,”
The staff of LGBTQ-friendly facilities may include specialists like Hutchinson-Colas, family doctors, physician assistants, nutritionists, infectious-disease specialists, endocrinologists, plastic surgeons, voice therapists and substance-abuse counselors, as well as behavioral-health specialists to address psychological issues.
A multitude of physical and emotional problems can arise from the stress of discrimination and identity issues. The LGBTQ population has the highest rates of tobacco, alcohol and drug use, including use of opioids. Lesbians and bisexual women are more likely to be overweight or obese. Gay men are at higher risk of HIV and other STDs, especially among communities of color. And LGBTQ youth are two to three times more likely than the general population to attempt suicide; they are also more likely to be homeless.
“The LGBTQ community has a higher risk for anxiety and depression,” says Dr. Todd Levin, medical director of Jefferson Health Primary and Specialty Care in Haddonfield, an LGBTQ-affirming practice. “There’s a lot of bias and discrimination, so it’s natural that individuals turn to ways to try to cope that unfortunately include substance abuse.”
When the practice opened in 2021, the transgender community, especially, had been putting off health care because of worry about bias, says Levin. “A big issue with transgender men is neglecting gynecological care,” he says. The practice began providing that service in June.
While the practice welcomes everyone, it caters to LGBTQ patients. A factor in opening the practice was the proximity to Collingswood. The borough has the fourth highest number of same-sex couples in New Jersey, according to the Williams Institute, which conducts research on sexual orientation and gender identity. “It’s very important to feel comfortable and have an open relationship with your provider,” says Levin.
Levin himself has been a member of the LGBTQ community for most of his life. “I initially found it difficult and challenging to discuss personal issues with my health care providers,” he recalls. “I wasn’t sure how they would feel about gay patients. It took awhile, but I’m glad to say I found a provider with whom I felt comfortable.”
Eleanor Gilman is a frequent contributor with a special interest in health and lifestyle issues.
