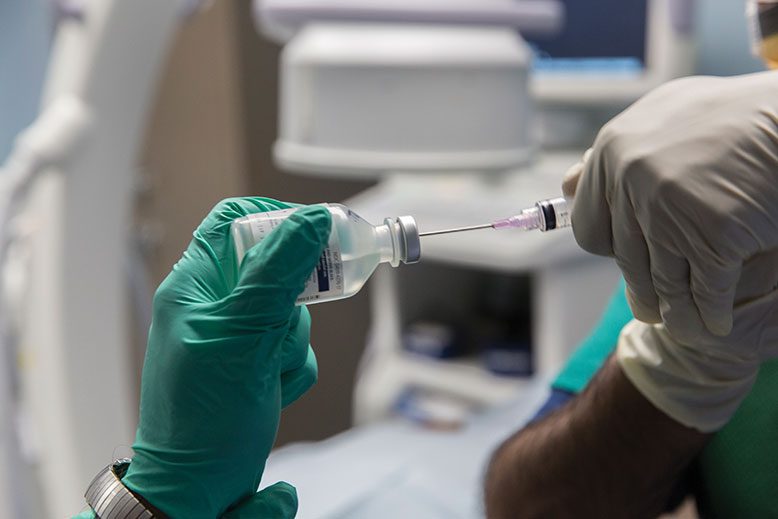
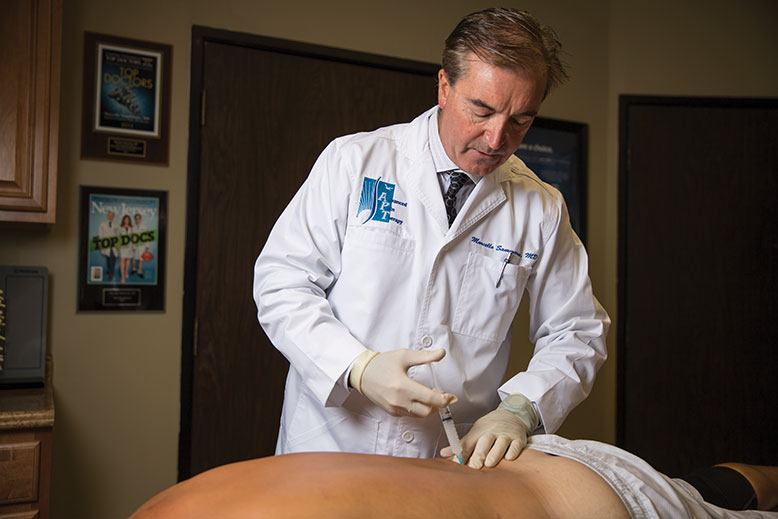
Dr. Marcello Sammarone, a pain-management specialist in Parsippany, administers a trigger-point injection to a patient with myofascial pain. The injections are quick, in-office procedures that require no sedation and soothe muscle spasms. Photo by Fred R. Conrad
Injections
After suffering on and off for nearly five years from sciatica—a condition in which a herniated (or bulging) disc presses on a nerve and sends pain radiating down the leg—Caryl Blank was willing to try anything, except opioids, to which she’d previously reacted badly. Her pain management specialist suggested a series of epidurals—pain-numbing injections into the area surrounding the spine. The Hackensack resident has had three epidurals so far, but the effect has been extremely short-lived. “I’m going back to see if there’s more my doctor can do,” she says, still hopeful.
In fact, injections don’t work for every patient, though when they do work, they can be quite effective, at least for a period of months. Pain specialists can utilize a variety of different injections, depending on the source of a patient’s pain. Epidurals are used to reduce pain emanating from the spine, particularly sciatica. Generally comprising an anesthetic and a corticosteroid, epidurals numb and reduce inflammation in affected nerves. Like epidurals, facet-joint injections treat spinal pain with a mixture of an anesthetic and a corticosteroid, but are administered into the space between vertebrae and used mainly to ease the pain of arthritic joints in the spine.
Trigger-point injections, on the other hand, treat the painful muscle knots known as trigger points and can also be used in the treatment of fibromyalgia and tension headaches. Containing a local anesthetic or saline, and sometimes a corticosteroid to reduce inflammation, the injections reduce pain by temporarily numbing and relaxing trigger points. (According to a 2013 Johns Hopkins study, adding fluid—saline or a local anesthetic—to the space around the spine sometimes relieves pain.)
None of these injections fix the conditions they target, but for many people, the shots—and similar procedures like corticosteroid injections for knee and other joint pain and sacroiliac joint blocks—offer several months’ relief. Dr. Chetan Malik, an assistant professor in Rutgers’s Department of Physical Medicine and Rehabilitation, says their major benefit, in addition to alleviating pain, is that they “provide patients with a window in which to bring other pain strategies”—cognitive behavioral therapy, physical therapy, exercise, and so on—“into the mix,” without the distraction of pain.
RadioFrequency Ablation
Another therapy for spinal pain, radiofrequency ablation (RFA) is a minimally invasive procedure, generally performed under a local anesthetic, that uses radio waves to cauterize affected nerves, temporarily disabling their ability to transmit pain signals. Its effect can last from 3 to 24 months. Other types of ablation use chemicals or extreme cold to achieve similar effects. This spring, the FDA approved Coolief, the first RFA treatment specifically for chronic knee pain caused by osteoarthritis.
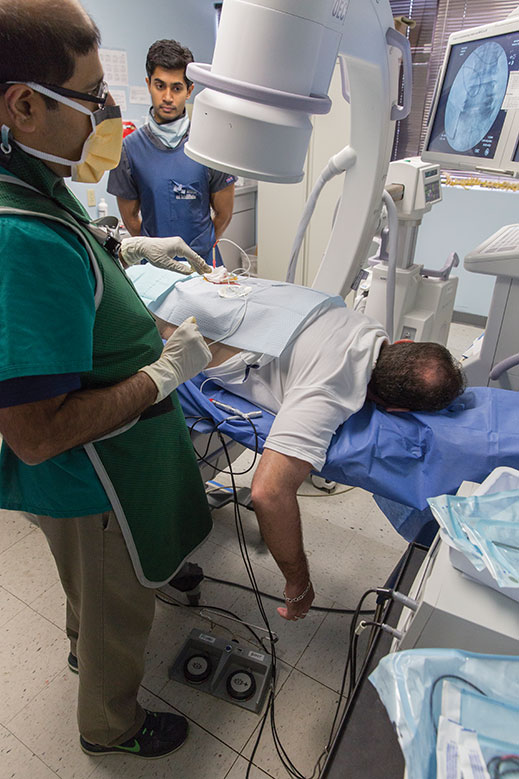
Dr. Chetan Malik of Rutgers New Jersey Medical School uses a fluoroscope to locate the area where a probe will deliver radio waves to cauterize a nerve. So-called radiofrequency ablation is effective in eliminating constant pain. Patients may not need another treatment for a year. Photo by Fred R. Conrad
Calmare Therapy
Four months after a botched podiatric surgery, Ridgewood resident Marilyn Green started to experience intense pain in her right foot. She was diagnosed with reflex sympathetic dystrophy (now largely known as complex regional pain syndrome type 1), a neurological disorder in which pain from damage to the soft tissues and/or peripheral nerves can spread to other parts of the body. Leery of narcotics, she self-prescribed a combination of B-complex vitamins and exercise that had proven beneficial to her mother after a case of shingles. The treatment offered some relief, but the gnawing pain persisted and began to spread. Green came across an article describing a rare procedure known as Calmare, designed to treat neuropathy, the nerve damage and concurrent chronic pain that can arise after chemotherapy, a shingles outbreak, or surgery. In cases like Green’s, says Michael Cooney, a chiropractor who is one of the few practitioners in the state to use the therapy, “we think there’s a hypersensitivity that’s developed within the pain center of the brain.” The Calmare device uses electrodes to move what Cooney calls “a no-pain signal” through the area of pain in order to “reboot” the brain, so that it’s no longer aware of the pain.
Cooney treated Green with 10 sessions of Calmare, and she is now pain free. “When I went in there, my pain level was at nine,” she says. “On day five of the treatments, it was down to zero.”
Calmare is effective only on true neuropathies; it appears to offer relief ranging from 6 to 18 months or longer.
Harnessing the Mind
The ways in which we perceive pain physically and emotionally are intimately connected in the brain, creating a delicate pas de deux in which emotional reactions can either limit our perception of pain or amplify it. Fear and anxiety, for instance, can intensify pain, while distracting the mind can ease it. That’s why so many multimodal approaches to pain management include cognitive behavioral therapy (CBT), whose goal is to change destructive thought patterns and devise positive coping strategies.
“It’s an active therapy, a collaborative approach between therapist and patient that encourages problem solving,” says Frank Sileo, a psychologist in Ridgewood. Through therapy sessions and homework (like deep-breathing exercises and journaling to track reactions to pain), patients learn to think differently about their pain.
CBT is often combined with mindfulness, a method of focusing attention on the present moment without judging it as either good or bad. One of the tenets of mindfulness, notes Sileo, is that “there’s pain, and then there’s suffering.” Pain, he says, is real, “but suffering is what we tell ourselves about that pain.” For pain patients, the goal of CBT and of mindfulness is to end the suffering by changing the story they tell themselves. In fact, a 2017 study out of King’s College London showed that acceptance and commitment therapy (ACT), a form of CBT incorporating mindfulness, significantly improved quality of life for patients suffering from chronic pain.
Medical doctors can also play a role in harnessing the mind’s power over pain. Dr. Lewis Nelson, chief of service at University Hospital’s emergency department in Newark, believes that the most significant effort in pain management may be the movement to manage patients’ expectations. “The fear of the unknown,” he says, “is greater than the reality of what is happening medically in most situations.” If a patient arrives at the ER, say, with a painful broken ankle, the treating physician should explain when the pain is likely to go away and what level of relief the patient is likely to receive from the medications or therapies that the doctor prescribes. If the doctor doesn’t offer this information, the patient should ask for it.




What about when you have tried everything
Trying to sit up and have coffee trying not to cry just watering eyes. As everyone else I’ve tried over counter things even sleeping pills! It did not put me to sleep I’m guessing because of pain. Told to try pot it’s been over 2 yes so why not friend came over said it was mild, I took 2 puffs could hardly walk to bed!! A lot of days can’t walk away, but I won’t do that again! Don’t know what they sell in pot stores but not for me! The meds for fibromyalgia does same thing.at lease with the pain pills I can get up and do things.didnt want to do the pot but as u know we or some will try anything. Not having good day hope this makes sense!! I think they health insurance companies are now over run with baby boomers and trying to save money don’t know how bad they will let us get before something is done could say more but got to go best to u and ur wife
I had 5 spine surgeries and one of mine failed I have two plates in my neck and one in my lower spine. I have pain 😫 everyday for ten years I don’t take narcotics although but other medications I take for pain but my health is not good due to chronic pain lost 48 pounds there is no help out there for some of us I want to know who is going to help us those who suffer being treated like a drug addict when your suffering bad it’s really sad.